
Myelopathy Musings: Walking Towards Healing
Amidst the recent struggles with my condition, a blend of January blues and the biting cold weather, my IBS has…

Amidst the recent struggles with my condition, a blend of January blues and the biting cold weather, my IBS has…

What is your name and where do you live? My name is Justin Michael Lantz and I live in sunny…
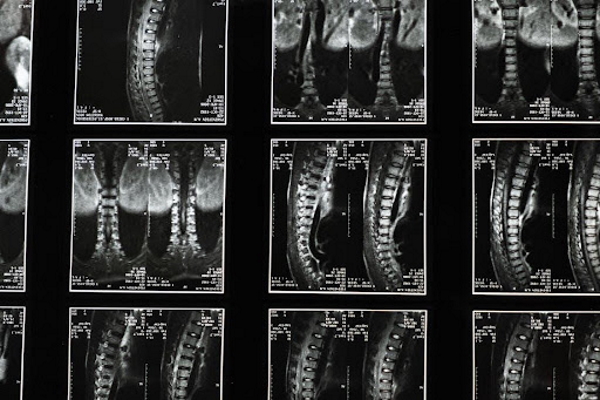
Although spinal cord compression (seen on MRI scans) is the dominant cause of degenerative cervical myelopathy (DCM), spinal cord stress…

Stepping into the Night On the Coffee Breaks this month we’ve been talking about what activities we’d love to try…

Exciting news! We are delighted to announce we are creating a stationery collection to support myelopathy awareness. It not only…

Part 1: Who Am I? My name is Gillian and I have lived independently with various cats and a very…

The gut microbiota is composed by trillions of bacteria, viruses, fungi, and archaea that contribute to maintaining homeostasis in our…

Overcoming Invisible Loneliness It’s so great that the Coffee Break group is providing support and addressing the challenges of loneliness…